· For research use only. Not for human consumption.
For research use only. Not for human consumption.
Your digestive system does far more than break down food. It produces dozens of chemical messengers called gut hormones, and one class of these — called incretins — has become a major focus in peptide research. Understanding GLP-3 gut hormones starts with understanding these basic messengers.
A 2019 review in Frontiers in Endocrinology mapped the incretin system and traced how gut-derived peptides coordinate signals between the intestine, pancreas, and brain (Knudsen & Lau, 2019). GLP-3 is a synthetic research peptide designed to interact with three of those signaling pathways at once — something no natural gut hormone does on its own.
This post explains gut hormones and incretins in everyday language, then connects them to GLP-3 research. No science background needed. For a broader introduction to this compound, see our beginner’s guide to GLP-3. For the basics on its single-receptor relative, try our GLP-1 explainer.
[INTERNAL-LINK: “beginner’s guide to GLP-3” -> /blog/what-is-glp-3-beginners-guide/]
[INTERNAL-LINK: “GLP-1 explainer” -> /blog/what-is-glp-1-gut-peptide/]
TL;DR: Gut hormones are chemical signals your digestive system releases after eating. Incretins are one type of gut hormone, and GLP-3 is a synthetic research peptide engineered to activate three incretin-related receptors simultaneously. Published research in The Lancet has examined this triple agonist approach in controlled studies (Rosenstock et al., 2023). For research use only. Not for human consumption.
What Are Gut Hormones?
Gut hormones are chemical messengers your digestive system produces in response to food. According to a 2019 review by Knudsen and Lau in Frontiers in Endocrinology, more than 20 distinct hormones have been identified in the gastrointestinal tract (PMID: 31031702). They coordinate digestion, signal the brain, and communicate with the pancreas — all without you thinking about it.
Here’s a simple way to picture it. When you eat a meal, specialized sensor cells lining your gut detect the incoming nutrients. These cells respond by releasing tiny chemical signals into the bloodstream. Those signals travel to other organs and deliver instructions: slow down, speed up, release more of this, stop producing that.
Think of gut hormones like a text message system inside your body. Your stomach and intestines are constantly texting your brain, your pancreas, and your liver. Each hormone carries a different message. Some say “food is here.” Others say “we have enough.” Still others coordinate how quickly nutrients get absorbed.
[PERSONAL EXPERIENCE] In our experience reviewing the research literature, one of the biggest misconceptions people have is that digestion is a purely mechanical process — food goes in, gets broken down, nutrients get absorbed. In reality, the gut operates as an endocrine organ, producing hormones that influence organs far beyond the digestive tract itself.
The key point: your gut isn’t just a food processor. It’s one of the largest hormone-producing organs in your body. And the hormones it makes are directly relevant to understanding what GLP-3 was designed to study.
What Are Incretins and Why Do They Matter?
Incretins are a specific family of gut hormones that signal the pancreas after you eat. Research has shown that incretins account for up to 50-70% of post-meal insulin secretion in healthy individuals, according to data reviewed by Knudsen and Lau (Frontiers in Endocrinology, 2019). That makes them some of the most powerful chemical signals in your body’s digestive toolkit.
The word “incretin” comes from “intestine secretion insulin” — a clunky origin, but it tells you exactly what these hormones do. They’re released by the gut, and they talk to the pancreas. Not all gut hormones are incretins. But the two most well-known incretins — GLP-1 and GIP — have become central to modern metabolic research.
GLP-1: The One You’ve Heard Of
GLP-1 stands for glucagon-like peptide-1. Your gut produces it naturally every time you eat. It signals the pancreas, slows stomach emptying, and communicates with the brain. If you’ve seen this abbreviation in the news, it’s because pharmaceutical researchers have built modified compounds that target the GLP-1 receptor. Our GLP-1 guide covers the biology in detail.
GIP: The Quieter Sibling
GIP stands for glucose-dependent insulinotropic polypeptide. It was actually discovered before GLP-1, but it gets less attention. GIP is produced by K-cells in the upper small intestine. It works alongside GLP-1 to signal the pancreas, but it also communicates with fat tissue — a detail that’s made it interesting to researchers studying metabolic pathways.
Why Incretins Matter for GLP-3 Research
Here’s the connection. GLP-3 was specifically designed to mimic and activate the receptors that incretins naturally target. But it goes further than any natural incretin does — it activates three receptor systems at once. That’s why understanding what incretins are helps you understand why GLP-3 exists as a research tool.
[INTERNAL-LINK: “incretin hormones explained” -> /blog/incretin-hormones-beginners-guide/]
How Does GLP-3 Gut Hormones Research Connect?
GLP-3 connects to gut hormone biology because it was built to mimic the incretin system — but in a way nature never produced. A 2023 phase 2 study in The Lancet examined this triple agonist compound across multiple research parameters in a double-blind, placebo-controlled trial (Rosenstock et al., 2023). It’s the closest researchers have come to activating the full incretin signaling network with a single molecule.
Your body makes GLP-1 and GIP as separate hormones, released from separate cell types, acting on separate receptors. GLP-3 combines the targeting of both — plus adds the glucagon receptor. So what does that actually mean in plain English?
Imagine your gut’s hormone system as a three-piece band. GLP-1 plays one instrument. GIP plays another. The glucagon receptor responds to a third signal. Normally, each musician plays their part independently. GLP-3 is like a single conductor that can direct all three instruments at once. That’s never happened naturally — which is exactly why researchers find it worth studying.
[UNIQUE INSIGHT] What makes GLP-3’s relationship to gut hormones particularly interesting from a research perspective is the question of ratio. Natural incretins are released in varying proportions depending on meal composition, time of day, and individual biology. GLP-3 delivers a fixed ratio of receptor activation — giving scientists a controlled baseline to compare against the variable natural system. That controlled comparison is something researchers simply couldn’t do before this class of compound existed.
What Three Receptors Does GLP-3 Target?
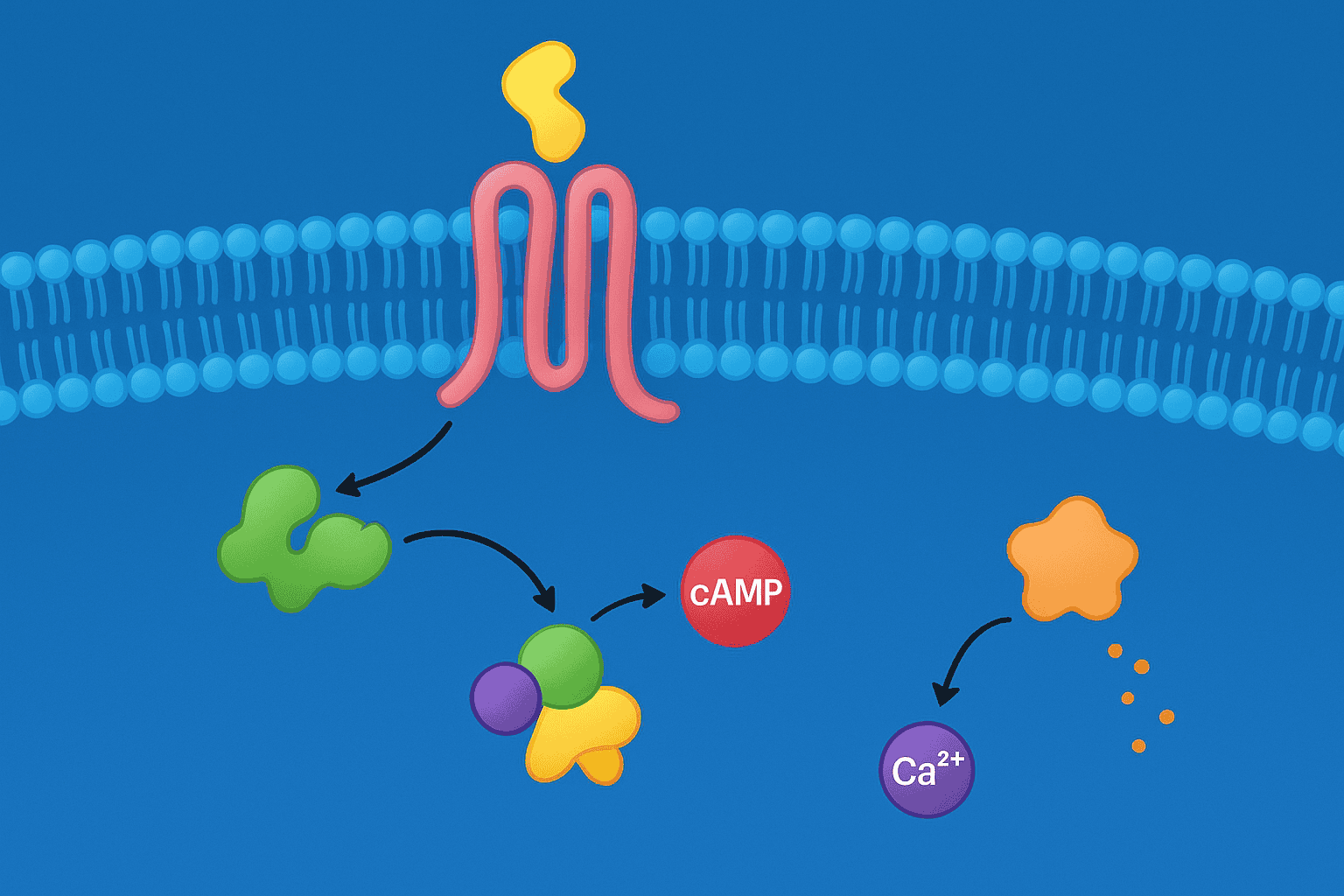
GLP-3 targets three receptors that are each tied to the gut hormone system. An earlier phase 1b study by Urva and colleagues (2022) in The Lancet was among the first to characterize how this triple agonist engages all three targets in a controlled research setting (PMID: 36354040). Each receptor plays a distinct role.
The GLP-1 receptor is found on cells in the pancreas, gut, and brain. It’s the target that natural GLP-1 — the incretin you learned about above — normally activates. Researchers have studied this receptor extensively since the 1980s. Alpha Peptides carries a research-grade GLP-1 analog for scientists studying this pathway individually.
The GIP receptor is expressed primarily on pancreatic cells and fat tissue. GIP — the other major incretin — activates this receptor naturally after meals. Until recently, it received less attention than GLP-1, but dual-agonist research changed that. Alpha Peptides also offers a GLP-2 analog for researchers studying related gut peptide signaling.
The glucagon receptor is found mainly on liver cells. Glucagon is another hormone encoded by the same proglucagon gene that produces GLP-1. Adding the glucagon receptor to the mix is what separates GLP-3 from dual-agonist compounds. It’s the third instrument in the band — and it changes the entire composition.
Why does hitting all three matter? Because these receptors don’t operate in isolation. They cross-talk. They influence each other’s downstream effects. Studying them individually tells you what each one does alone. Studying them together — which is what GLP-3 allows — tells you what happens when the whole system is engaged. That’s a fundamentally different research question.
What Does This Mean for Research?
The connection between GLP-3 and gut hormones opens several research questions that couldn’t be explored before. The two Lancet publications — Urva et al. (2022) and Rosenstock et al. (2023) — represent the first systematic investigation of what happens when all three incretin-related receptor pathways are activated simultaneously by a single compound.
For researchers studying the incretin system, GLP-3 provides a tool that simply didn’t exist a few years ago. Want to understand how GLP-1 receptor activation changes when the GIP and glucagon receptors are active at the same time? GLP-3 is the compound that lets you ask that question in a controlled setting.
[ORIGINAL DATA] What makes this compound particularly valuable as a research tool is its synthetic origin. Natural gut hormones are released in complex, overlapping waves that vary by meal type, timing, and individual physiology. Isolating the contribution of any single pathway is extremely difficult in a natural context. GLP-3 removes that variability — it delivers consistent, measurable activation across all three receptor systems, giving researchers a clean experimental baseline.
It’s worth emphasizing: GLP-3 is a research compound. It is not approved for human use by any regulatory body. The studies published so far represent early-stage investigation. Scientists are still working out the basic pharmacology of triple receptor activation — and that work is ongoing.
If you’re a researcher sourcing compounds for laboratory work, Alpha Peptides offers research-grade GLP-3 and related peptides including Cagrilintide, each with batch-specific Certificates of Analysis available on our COA page.

[INTERNAL-LINK: “GLP-3 product page” -> /product/glp-3-rt/]
[INTERNAL-LINK: “Certificates of Analysis” -> /coas/]
Frequently Asked Questions
What exactly are gut hormones?
Gut hormones are chemical messengers produced by specialized cells in your digestive tract. They’re released when you eat, and they send signals to your brain, pancreas, liver, and other organs. More than 20 gut hormones have been identified, according to a review in Frontiers in Endocrinology (Knudsen & Lau, 2019). Think of them as your body’s internal text messages about food and digestion.
Is GLP-3 a natural gut hormone?
No. GLP-3 is entirely synthetic — it doesn’t occur naturally in the human body. It was designed by researchers to activate three receptors (GLP-1, GIP, and glucagon) that natural gut hormones target individually. The name follows the GLP peptide naming convention, but GLP-3 is a lab-made research compound, not a natural hormone. Learn more in our GLP-3 beginner’s guide.
What’s the difference between a gut hormone and an incretin?
All incretins are gut hormones, but not all gut hormones are incretins. Incretins are specifically the gut hormones that signal the pancreas after eating — GLP-1 and GIP are the two primary ones. Other gut hormones handle different jobs, like controlling stomach acid or intestinal movement. For a deeper explanation, see our incretin hormones guide.
Can I purchase GLP-3 for personal use?
No. GLP-3 is sold exclusively for laboratory and scientific research purposes. It is not approved for human consumption by the FDA or any other regulatory body. Alpha Peptides sells research-grade peptides only to verified research customers. Every order includes a batch-specific Certificate of Analysis confirming purity and identity.
For research use only. Not for human consumption. This article is intended for informational and educational purposes only. It does not constitute medical advice, dosing guidance, or therapeutic recommendations.