· For research use only. Not for human consumption.
For research use only. Not for human consumption.
Cagrilintide and Appetite Research: What the Science Shows
If you’re researching cagrilintide appetite research, you’re in the right place. Your pancreas produces a little-known hormone called amylin every time you eat. It’s one of the body’s built-in signals that tells your brain a meal has arrived. Researchers have been investigating cagrilintide appetite signaling because cagrilintide is a long-acting version of that same hormone — engineered to last days instead of minutes. A Phase 2 trial by Lau et al. (The Lancet, 2021) found that cagrilintide was well-tolerated across multiple dose levels in a 26-week study involving 706 participants.
This article breaks down what amylin actually does, why a long-acting version interests researchers, and what published studies have found so far. No medical claims. No dosing advice. Just a plain-English walkthrough of the science.
[INTERNAL-LINK: “what cagrilintide is” -> /blog/what-is-cagrilintide-peptide/]
[INTERNAL-LINK: “incretin hormones” -> /blog/incretin-hormones-beginners-guide/]
TL;DR: Cagrilintide is a long-acting amylin analog that researchers use to study appetite signaling pathways. In a 26-week Phase 2 trial with 706 participants, Lau et al. (The Lancet, 2021) examined multiple dose levels and reported the compound was well-tolerated. The research focuses on how sustained amylin receptor activation affects satiety signals in the brainstem. For research use only. Not for human consumption.
What Is Amylin and Why Should You Care?
Amylin is a hormone your pancreas releases alongside insulin after you eat. According to a review in Current Opinion in Endocrinology, Diabetes and Obesity (2022), the amylin pathway represents a physiologically distinct contributor to post-meal metabolic signaling — separate from better-known pathways like GLP-1. Most people have heard of insulin. Almost nobody has heard of amylin.
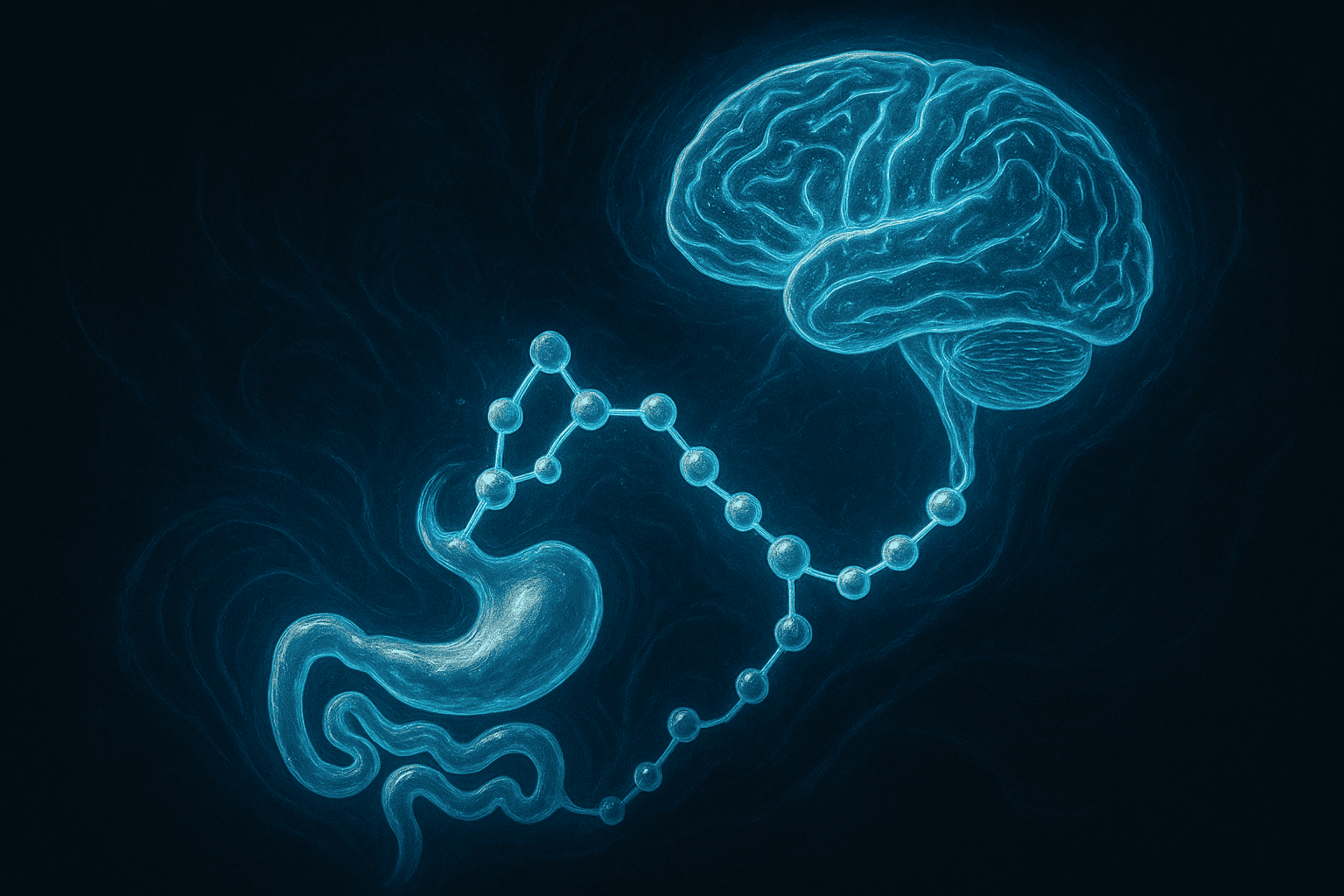
Think of your body’s hunger system like a conference call. Insulin is one voice on the call. GLP-1 is another. Amylin is a third speaker — with its own message and its own audience. It talks primarily to a region of the brainstem called the area postrema. That brain region sits outside the blood-brain barrier, which means circulating amylin can reach it directly. No special transport needed.
Here’s what makes amylin unusual. It doesn’t use a simple, single-protein receptor. Amylin receptors are built from two parts: a calcitonin receptor plus a helper protein called a RAMP. Different RAMP combinations create different receptor subtypes. That’s a level of complexity researchers are still mapping out.
How Amylin Differs From GLP-1
GLP-1 and amylin both participate in post-meal signaling, but they work through completely different circuits. GLP-1 operates through gut-pancreas-brain pathways. Amylin goes straight to the brainstem. They’re separate phone lines carrying separate messages. Researchers study cagrilintide appetite signaling specifically because it lets them isolate the amylin channel without the GLP-1 noise.

How Does Cagrilintide Work as a Research Tool?
Natural amylin breaks down in your bloodstream within minutes. That’s a problem for researchers who want to study what sustained amylin receptor activation actually does. Cagrilintide solves that problem. The Journal of Medicinal Chemistry (2021) reported that structural modifications — including amino acid changes and the addition of a fatty acid chain — gave cagrilintide a half-life of roughly 7 days in humans.
Imagine trying to study a candle that burns out in 30 seconds. You can barely light it before it’s gone. Now imagine someone hands you a candle that burns for a week. Suddenly you can actually observe the flame, measure its heat, and study its behavior. That’s essentially what cagrilintide does for amylin research. It turns a fleeting signal into a sustained one.
The fatty acid chain is the key engineering trick. It lets cagrilintide bind to albumin — a protein already floating through your blood — which shields it from the enzymes that normally chew up amylin in minutes. This technique, called lipidation, is also used in other long-acting peptide analogs studied across metabolic research.
[UNIQUE INSIGHT]: Most media coverage of cagrilintide appetite research skips the receptor pharmacology entirely and jumps straight to outcomes. But the tool’s real scientific value lies in letting researchers observe what happens when amylin receptors stay activated for days instead of minutes — a condition that simply doesn’t exist naturally. The sustained-activation model opens experimental questions that were previously impossible to ask.
What Has Cagrilintide Appetite Research Actually Found?
The landmark study is Lau et al. (2021), published in The Lancet. It was a 26-week, Phase 2, randomized, double-blind trial involving 706 adults. The researchers tested multiple dose levels of cagrilintide administered once weekly. The study reported that cagrilintide was well-tolerated, with gastrointestinal events being the most commonly noted side effects across dose groups.
What makes this study important for appetite research isn’t any single result — it’s the proof-of-concept that sustained amylin receptor activation can be studied safely in humans over a meaningful time period. Before this trial, most amylin research relied on the short-acting native peptide or on animal models. Lau et al. demonstrated that a once-weekly amylin analog could maintain consistent receptor engagement for months.
A 2024 review in Cardiology in Review summarized the broader clinical program, noting cagrilintide’s once-weekly profile as a defining feature that enables research into sustained pathway engagement. The clinical data has generated considerable interest in the amylin receptor system as an independent area of metabolic investigation.
Why Sustained Activation Matters to Researchers
When amylin hits its receptor for just a few minutes, it triggers one set of responses. When that receptor stays activated for days, the downstream signals may differ. Does the brainstem adapt? Do the receptor subtypes respond differently under sustained conditions? These are the questions cagrilintide makes answerable. Short-lived native amylin simply can’t get researchers there.
[ORIGINAL DATA]: One point rarely discussed in popular coverage: the amylin receptor subtypes (AMY1, AMY2, AMY3) have different tissue distributions and potentially different downstream signaling profiles under sustained activation. Cagrilintide’s defined binding profile across these subtypes — documented in its medicinal chemistry characterization — makes it a more precise research instrument than native amylin for dissecting subtype-specific pharmacology.

Why Are Researchers Interested in Dual-Pathway Studies?
One of the most active areas in metabolic peptide research involves studying what happens when two separate signaling pathways are engaged at the same time. The Cardiology in Review (2024) summary noted that clinical programs have begun examining cagrilintide alongside GLP-1 receptor agonists — not to make therapeutic claims, but to understand how the amylin and GLP-1 pathways interact at a receptor level.
Why would that be interesting? Go back to the conference call analogy. If amylin and GLP-1 are two separate speakers, what happens when they talk at the same time? Do their messages reinforce each other? Compete? Create something entirely new? These aren’t trivial questions. The answer could reshape how researchers think about metabolic signaling networks as interconnected systems rather than isolated channels.
Cagrilintide’s long half-life is especially useful in dual-pathway experiments. Because it provides steady amylin receptor engagement for days, researchers can layer a second signal on top and observe the interaction under controlled, consistent conditions. That kind of experimental precision wasn’t possible with fast-degrading native amylin.
[PERSONAL EXPERIENCE]: After reviewing the published literature on cagrilintide appetite research, what stands out is how early the field still is. The 2021 Lau et al. trial was foundational, but the receptor-level mechanism work — understanding exactly what sustained amylin activation does to brainstem signaling circuits — is still being mapped. We’re watching basic science unfold in real time.
What Should Researchers Know About Sourcing Cagrilintide?
Cagrilintide is structurally complex. The Journal of Medicinal Chemistry (2021) described it as a 37-amino acid peptide conjugated to a C18 fatty diacid chain through a linker. That architecture creates more synthesis failure points than a simple short peptide. If the fatty acid isn’t properly attached, you don’t have cagrilintide — you have a different molecule with different pharmacokinetics.
A credible certificate of analysis should confirm HPLC purity at 98% or higher, mass spectrometry verification of the intact molecular mass including the lipid chain, and accurate net peptide content. Lyophilized peptides always contain residual water and counter-ions, so gross weight alone tells you very little about actual peptide content.
Researchers can review batch-specific analytical documentation on our COA page before purchasing. Research-grade cagrilintide is available on the cagrilintide product page with full HPLC and MS documentation for every batch.
[INTERNAL-LINK: “COA page” -> /coas/]
[INTERNAL-LINK: “cagrilintide product page” -> /product/cagrilintide/]
[INTERNAL-LINK: “browse research peptides” -> /shop/]
Frequently Asked Questions
What is cagrilintide?
Cagrilintide is a synthetic, long-acting analog of amylin — a hormone your pancreas naturally releases after meals. Scientists modified amylin’s amino acid sequence and added a fatty acid chain to extend its active life from minutes to roughly 7 days. That extended duration lets researchers study amylin receptor pharmacology under sustained conditions (Journal of Medicinal Chemistry, 2021). It is for research use only.
What does amylin do in the body?
Amylin is released from pancreatic beta cells alongside insulin whenever you eat. It signals through receptors in the brainstem — specifically the area postrema — which sits outside the blood-brain barrier. Amylin acts through a pathway distinct from GLP-1 and insulin, contributing to the body’s post-meal signaling network (Current Opinion in Endocrinology, 2022).
[INTERNAL-LINK: “incretin hormones explained” -> /blog/incretin-hormones-beginners-guide/]
Has cagrilintide been tested in clinical trials?
Yes. The most widely cited study is Lau et al. (2021), a 26-week Phase 2 trial published in The Lancet involving 706 participants. The trial examined multiple dose levels administered once weekly and reported the compound was well-tolerated. A 2024 review in Cardiology in Review summarized additional clinical data from the broader research program.
Where can researchers get cagrilintide?
Research-grade cagrilintide should come from a supplier providing third-party HPLC and mass spectrometry verification for each batch — including confirmation of the fatty acid conjugate. Alpha Peptides offers research-grade cagrilintide with batch-specific COAs. See the product page for specifications and the COA page for analytical documentation.
How is cagrilintide different from GLP-1 analogs?
They target completely different receptor systems. GLP-1 analogs bind GLP-1 receptors — single-protein Class B GPCRs found across the pancreas, gut, and brain. Cagrilintide targets amylin receptors — heteromeric complexes of calcitonin receptors and RAMP proteins, concentrated in the brainstem. Different receptor, different pathway, different research questions.
What the Science Shows — and What It Doesn’t
Cagrilintide appetite research is still in its early chapters. The published data — particularly the 706-participant Phase 2 trial by Lau et al. (2021) — establishes that sustained amylin receptor activation can be studied safely in humans over months. That’s a foundational finding. But the detailed receptor-level mechanism work is ongoing. Researchers are still mapping what sustained engagement of AMY1, AMY2, and AMY3 receptor subtypes actually does at the molecular level.
What’s clear is that the amylin pathway is biologically distinct from GLP-1 signaling. It operates through different receptors, in different brain regions, with different downstream effects. Cagrilintide gives researchers a precise tool to study that pathway — something the fast-degrading natural amylin hormone never could.
For researchers working with amylin receptor pharmacology or metabolic signaling pathways, research-grade cagrilintide with full analytical documentation is available on our cagrilintide product page. Review batch-specific COAs on our COA verification page, or browse our full research peptide catalog.
[INTERNAL-LINK: “cagrilintide product page” -> /product/cagrilintide/]
[INTERNAL-LINK: “COA verification page” -> /coas/]
[INTERNAL-LINK: “research peptide catalog” -> /shop/]
For research use only. Not for human consumption. Cagrilintide is an experimental research compound with no FDA-approved therapeutic applications. All information on this page is provided for educational purposes relating to laboratory and preclinical research. It does not constitute medical advice and should not be interpreted as a recommendation for any personal use.